- G. Bertazzoni
- Brief Report and Case Report
Simulation as a Didactic Method in Emergency Medicine
- 3/2016-Ottobre
- ISSN 2532-1285
1: President SIMEUP
* Emergency Medicine, NorthShore University Health System, Evanston, Illinois, USA
** (Research Center on Evaluation of Quality in Medicine – CEQUAM, “Sapienza” University Rome, Italy: D. Amoroso, L. Antonetti, M De Filippo, A. Garramone, I Gentile, A Marcellino, E Migliozzi, O Spagnolello, A Zizzo)
Abstract
Simulation is a teaching method that has witnessed a growing development in the last few years, especially in the fields of emergency medicine and critical care. To date, however, we lack a shared model of simulation, as well as a common framework for the management of debriefing and, more importantly, for the assessment of participants. But in order to rationally tackle these issues, we need to know the state of the art of simulation. The present article aims at presenting the existing simulation models, highlighting their differences while specifying possible recipients and applicative contexts.
The recent thrust of technology that has been experienced in recent years, as well as a marked increase in globalization (which also comes to pass through the flux of migration as well) are two phenomena which have directed the evolution of medicine towards greater complexity, and the ability to further highlight inequalities in public health. In reality, even the medical student has changed in current times: the classic lessons captures their attention for a shorter period of time in comparison with the past, and after twenty minutes a decay of the capacity to concentrate begins. Therefore, the possibility of comprehension decays along with it. Now new contemporary stimuli allow the student to better retain the information, which, more than merely assimilated, become stored and available for use at the moment of need. This is one of the motives for which Universities in Italy are rethinking the formation of medical education through a new teaching methodology, with the purpose of training mature professionals capable of providing a suitable response to current public health needs. This response would be nationally uniform, and in accordance with international development.
These premises pave the way for new scenarios: in the clinical setting, if knowledge is the base of understanding, knowledge may then become the base for the development of clinical competencies. This process must already be initiated as early as the undergraduate period within the various institutions of medical education (the introduction of the graduate advisor accelerates this process). A series of changes have been introduced in recent times within university didactics, however in a non-homogenous and overly institution-specific manner.Additionally, certain areas encountered in real situations may be difficult to teach in a classroom setting. Amongst these are the management of the patient and the awareness of human error, topics for which, from the didactic point of view, the employment of simulation becomes useful and advantageous.
Simulation is a didactic method which has had rapid growth in recent years, and which unites the interests of students, residents, and professionals in their shared endeavors to develop clinical competency in patient care. Those competencies comes from a base of theoretical knowledge (acquired from literature), and are developed through experience (procedural abilities), personal motivation, and consciousness (of the environment, decisional processes, and of human error). Ultimately, this inspires teamwork, with the awareness that many expert individuals are not the equivalent of an expert team (1), and that in a team, efficacious communication is one of the cardinal requirements in successful treatment. The didactic initiatives which utilize simulation as their method are growing; that which is still lacking is a common model of simulation. To achieve this, we must first think forward to a rational systematization of the topic.
Procedural simulations exist which utilize partial models and devices, and aim to teach procedural techniques and maneuvers. These skills, or “the ability to do something well”, are measured according to three levels – “see one, do one, teach one.” The levels depend on the level of education of the operator, generally students of medicine and health sciences. Safetyconcerns impede practicing invasive maneuvers directly on patients, and simulation allows practical teaching without risk to said patients (2). It is this ill-defined simulation setting on which we rely for all complex technical and procedural competence training (3). Instruction should be based on validated international protocol. The content should be identical regardless of who is teaching the course so that training will always be equal. The result is better if the student demonstrates enthusiasm in the simulation setting. The content of the teaching is freely transferred by the instructor, but favored by a facilitator. In the university setting, The Procedure Lab is brought for the sixth year students of the integrated course in Emergency Medicine and Surgery, the last chance before graduation, to gain experience with oropharyngeal airways, ambu-bags, defibrillators, endotracheal tubes, vascular access including ultrasound guided, intraosseous lines, etc. Devices for these partial simulations include: model heads for orotracheal intubation and needle tracheostomy; various instruments for ventilation techniques for adults and children; LMAs; model arms for vascular access including ultrasound guided, and intraosseous devices (needles and drills); external automatic defibrillators (EAD); monitors for defibrillation and cardioversion, transcutaneous pacemaker. As part of this skill set, one may acquire a BLS competency certificate through study of a manual and a formal activity done by certified instructors, in a relationship well defined between student and professor (in the role of facilitator of learning).
We have trained sixth year medical students with these low-tech simulation systems at the faculty of medicine at La Sapienza di Roma, while BLS-AHA certification is obtained by all students in their second year of study, and students in the health sciences and basic medical sciences. This is a first level of partial simulation designed for a cohort of students who will be able to learn competencies and procedures.
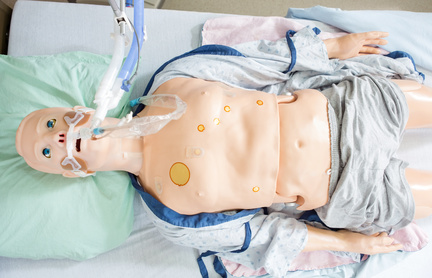
At another level is high-fidelity simulation; simulation of clinical cases, simulation that looks to teach the management of the case through trial and error; simulation which teaches the principal of CRM (crisis resource management) and teamwork, simulation which requires a mannequin (full body, not partial) and higher technology (complete with software to reproduce heart tones and respirations, to display vital signs on a monitor, and to reproduce images, if and when possible), which produces high fidelity scenarios (importance of the “director,” the “facilitator,” the “distractor” and individual team roles: team leader, the individual assigned to manage the monitor, the individual assigned to the airway, to the medications, and to CPR (during assigned intervals).
Every simulation assumes the existence of a case (problem) to solve. The best thing is always to choose real patient cases: in this way one may utilize all of their physical exam and lab values; diagnostic imaging, and one can tell a real story that developed with a patient. The key concepts are: prepare and bring the environment alive (including use of sound); simulate emotions, times and roles (challenges: unexpected equipment failure; perfecting the moulage, recollection of the script); personal external imagination; pacing of the scenario: not too fast, not too slow.
The scenario, reproduced with fidelity and realism, starts with the title and objectives as relayed by the author in the script, with regard to the type of student as well; it assumes a life-like atmosphere (moulage and instrument), with the presence of actors as well; a clinical case to recount, a partitioning of roles, management of the case; the director introduces the simulation, asks to identify specific roles, and then priorities and key points; the discussion begins; filling in if there are extended silences; analyzing the situation; encouraging discussion; adaptation of the facilitation to the groups abilities; using short interventions; at the end operates a summary of the debriefing, through which problems are analyzed, including those which needed assistance, interpersonal communication and work flow issues; and of application of guide lines and protocols.
The objective of debriefing is to promote critical reasoning by reexamining the scenario (3). Its success is bound to the ability of the “facilitator” in stimulating constructive criticism which can mature the experience. Debriefing can be problematic because of the lack of uniformity in its management (times of progressions and content; scope). Evaluation (individual and team performance; evaluation of single skill and general performance, also understanding the evaluation of communication between single components of the team) awaits systematization; the discussion of the following themes remains open: median times of duration of the scenario; quantity and quality of the pathologies of the adult and the child utilized to define a course of simulation.
The evaluation performed on single components of the team seem closer to an evaluation of “milestones” imparted on residents, such as annual in-service and end of year exams. Here particular milestones are considered, some of which will be included, such as: emergent stabilization; observation and re-evaluation of high acuity patients; diagnostic investigations; knowing how to cover various roles in an efficient manner for management of patients in the emergency department; general approach to procedures; airway management; anesthesia in the acute pain setting: sedation procedures and anesthesia on patients of any age in critical situations; use of technology in the approach to the patient; management of a team (4, 5, 6).
At this point the cultural base is such that it can be thought that the course doesn’t teach the pathology, but the management of the pathology, and could serve to change the daily modus operandi, and facilitating work in teams, use of guidelines, awareness of the environment (scenario) and the culture of error. Debriefing represents the moment of taking in conscious comprehension. This is a higher level of real simulation whose appropriate direction is professionals and high level residents. Learners are exposed to levels of difficulty tailored to their education level and various learning strategies (2).
- Burke CS, Salas E,Wilson-Donnelly K, Priest H : How to turn a team of experts into an expert medical team: guidance from the aviation and military communities. Qual Saf Health Care 13:i96–i104, 2004
- A. Ganau e Gruppo di lavoro Simulazione didattica La Simulazione nei Corsi di laurea in Medicina e Chirurgia italiani Med Chir. 70 3181-3183, 2016
- Santalucia P, Ingrassia PL, Zaninelli A, Ragazzoni L, Ganau A, Gensini GF: La simulazione in Medicina Med. Chir. 70. 3166-3169, 2016
- Dieckmann P, Friis SM, Lippert A, Østergaard D : The art and science of debriefing in simulation: ideal and practice. Med Teach 31:e287–e294, 2009
- Holmboe ES, Sherbino J, Long DM, Swing SR, Frank JR: The roleof assessment in competency-based medical education Med Teach 32 (8); 676-82 , 2010
- Frank JR, Snell LS, Cate OT et al Competency-based medical education: theory to practice Med Tech 32 (8) 638-45, 2010

